When you’re waiting to learn whether or not you have cancer, it’s fairly easy to assume the worst.
Everyone knows someone whose life has been touched by cancer – and there’s no escaping the many factors that leave us at an increased risk of developing the chronic disease. The risk is in the water we drink, the food we eat, the air we breathe and the rays of sun that kiss our face in the mornings.
More than two million Americans are expected to be diagnosed with skin cancer – the most common type of cancer – and over 626,000 are projected to die from it this year alone, according to the American Cancer Society.
All of these statistics add up to a fairly good chance of developing skin cancer, along with my history of running outside, my love of going to the beach, my glasses of wine with dinner and my consumption of Cheetos, which are laced with brightly-colored food dyes.
But what was swirling around in my head as I waited for the results of my biopsy last December wasn’t what I did wrong, it was what I had yet to do, what I would have to face and, above all, how to tell my parents over the Christmas holiday.
The team at NYU Langone Health’s Perlmutter Cancer Center was concerned enough about the mole on my left cheek to scoop it out of my face.
If they said that the sample showed what I feared was the beginning signs of melanoma – the deadliest form of skin cancer, affecting an estimated 112,000 this year – my life would likely have to change very quickly.
I’d felt more tired than usual, but that could be due to a host of issues. Although this wasn’t my first scare. I’d had cells that were weird in my cervix in previous years.
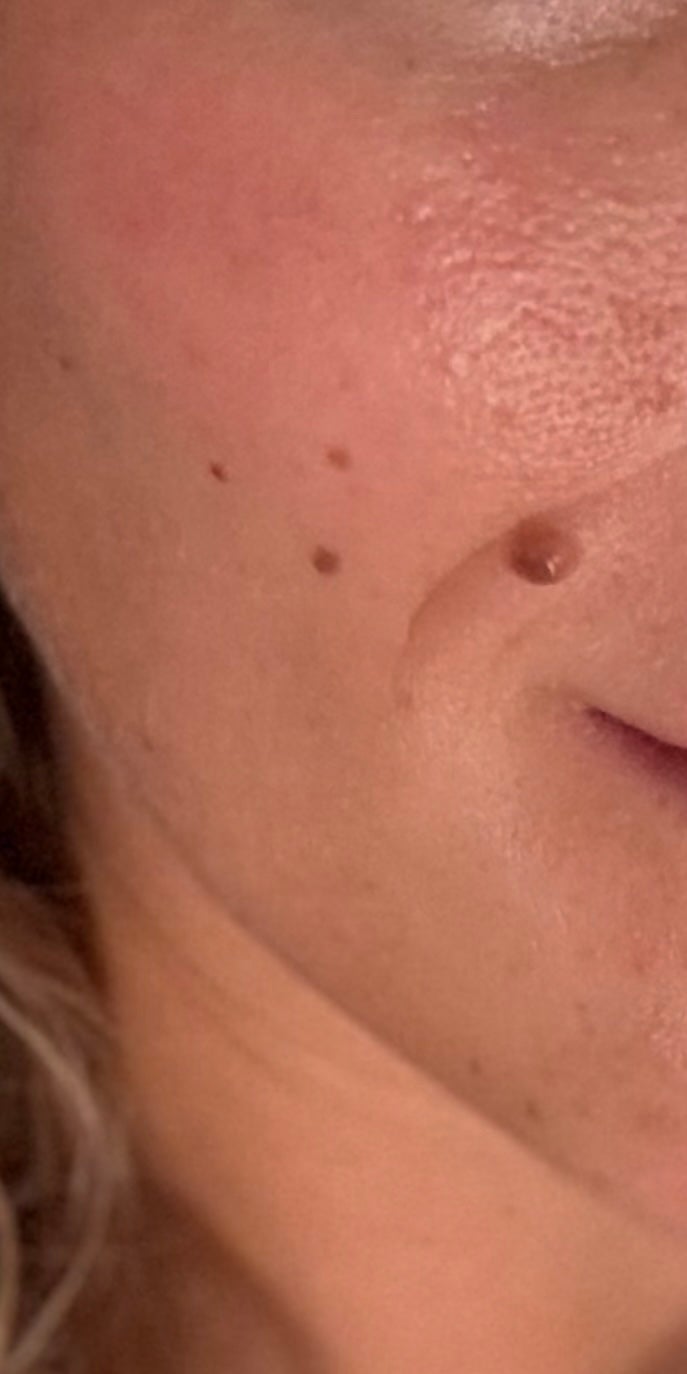
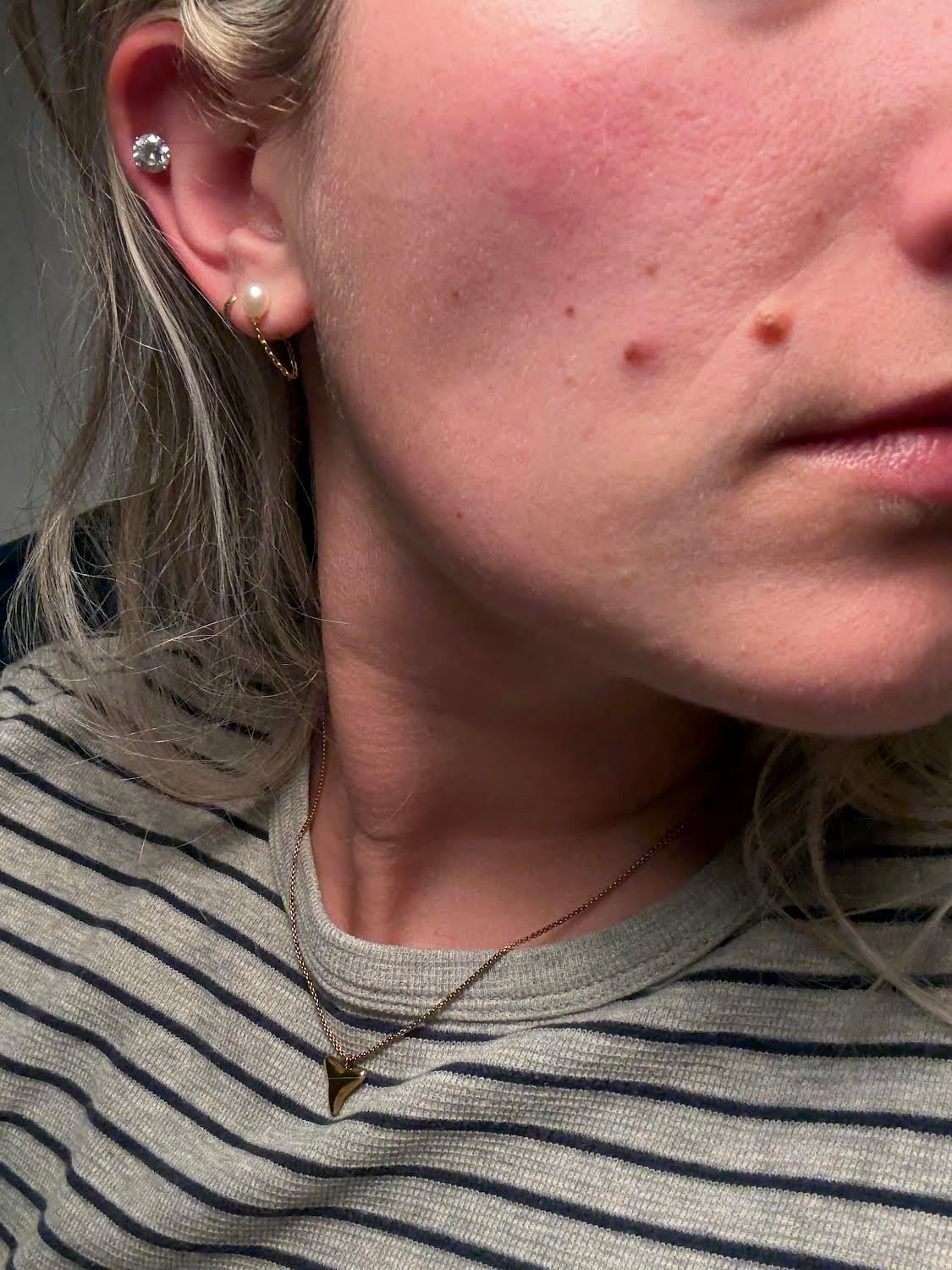
I started making small lifestyle changes after first noticing that the mole had changed, growing and darkening in color and beginning to itch, scab and hurt.
Even though it was around Thanksgiving, I stopped drinking alcohol, was eating more whole foods, drinking more water and getting more sleep.
Obviously, that wouldn’t reverse the suspected cancer; only treatment or surgery could eradicate it, if we had caught it early enough. But maybe it would help keep the rest of my body as healthy as possible while I fought the effects of melanoma.
I got the call on the way out the door of my office about a week after the biopsy. The cells from the mole were not quite melanoma, but had features that could lead to it.
My doctor said not to worry, and to monitor the area. We would check back in a year, unless the area started to change again.
It was a relief – but not quite as relieving as if the whole thing had just been a mistake – even with the hole in my face.
I got lucky. Yet, an estimated 46,600 women will be diagnosed with melanoma in 2026. Some 8,510 people are anticipated to die of the disease, the American Cancer Society says.
While rates have declined by one percent a year in men younger than 50, the rates have been stable among women. This is because the female hormone estrogen triggers the production of melanin-making cells, women use tanning salons more than men and women also get screened more than men.
Beyond just being a woman, having red hair and fairer skin is also a major risk factor. Although all types of skin are at risk from dangerous UV radiation, the Skin Cancer Foundation said in a link shared with The Independent.
Legendary Jamaican musician Bob Marley died from melanoma in 1981 at age 36.
Working outside, getting a sunburn, having a family history of melanoma or having an organ transplant also put people at a greater risk.
Organ transplant patients are at up to a 100 times higher risk for developing skin cancer compared to others because they are on medications that suppress the immune system, UCSF Health notes.
And though both tanning beds and the sun are sources of harmful ultraviolet radiation that can damage skin cell DNA and cause cancer – tanning beds are much worse. They emit around 12 times more radiation than the sun, raising the risk of developing malignant melanoma by 75 percent, according to UnityPoint Health.
Still, it only takes 15 minutes to damage skin, Hartford Heathcare says, and the risk increases as we age. The average age of people diagnosed with melanoma is 66, the society notes, and the foundation says that 20 percent of Americans will develop skin cancer by age 70.

I don’t have a family history of melanoma and I’ve never had an organ transplant, but I’ve definitely had one of those painful, lobster-red sunburns and I train for races along New York City’s Hudson River during the summer. Water reflects UV rays like a mirror, meaning that you’re being exposed from above and below.
When skin cancer is detected early, 99 percent of patients are alive for five years following diagnosis, the foundation says.
So people should examine their skin once a month, looking for any mole or growth that has increased in size and appears tan, brown, black, multicolored or pearly. An open sore that does not heal within three weeks can be a sign of skin cancer, as well as a spot that continues to itch, crust, scab, hurt or bleed.
Some signs of cancer could also be lurking under nail polish or hair – as well as in areas that don’t see any sun – so people at a higher risk for skin cancer should also see a doctor.
“We encourage everyone to make skin self-exams a regular habit including checking your skin regularly and talking with your doctor about any persistent changes,” Dr. Laura Makaroff, Senior Vice President of Prevention and Early Detection at the American Cancer Society, said in a statement shared with The Independent. “Catching changes early can make all the difference.”

